Why Pain Location Rarely Reveals the Real Problem
Pain has a frustrating habit of lying about where it comes from.
Your knee aches after a run. You rest it, ice it, maybe get some treatment. It feels better. Then two weeks later, same spot, same problem.
Or worse—the knee feels fine, but now your hip hurts.
This isn't bad luck. It's your body telling you that treating the location missed the actual problem.
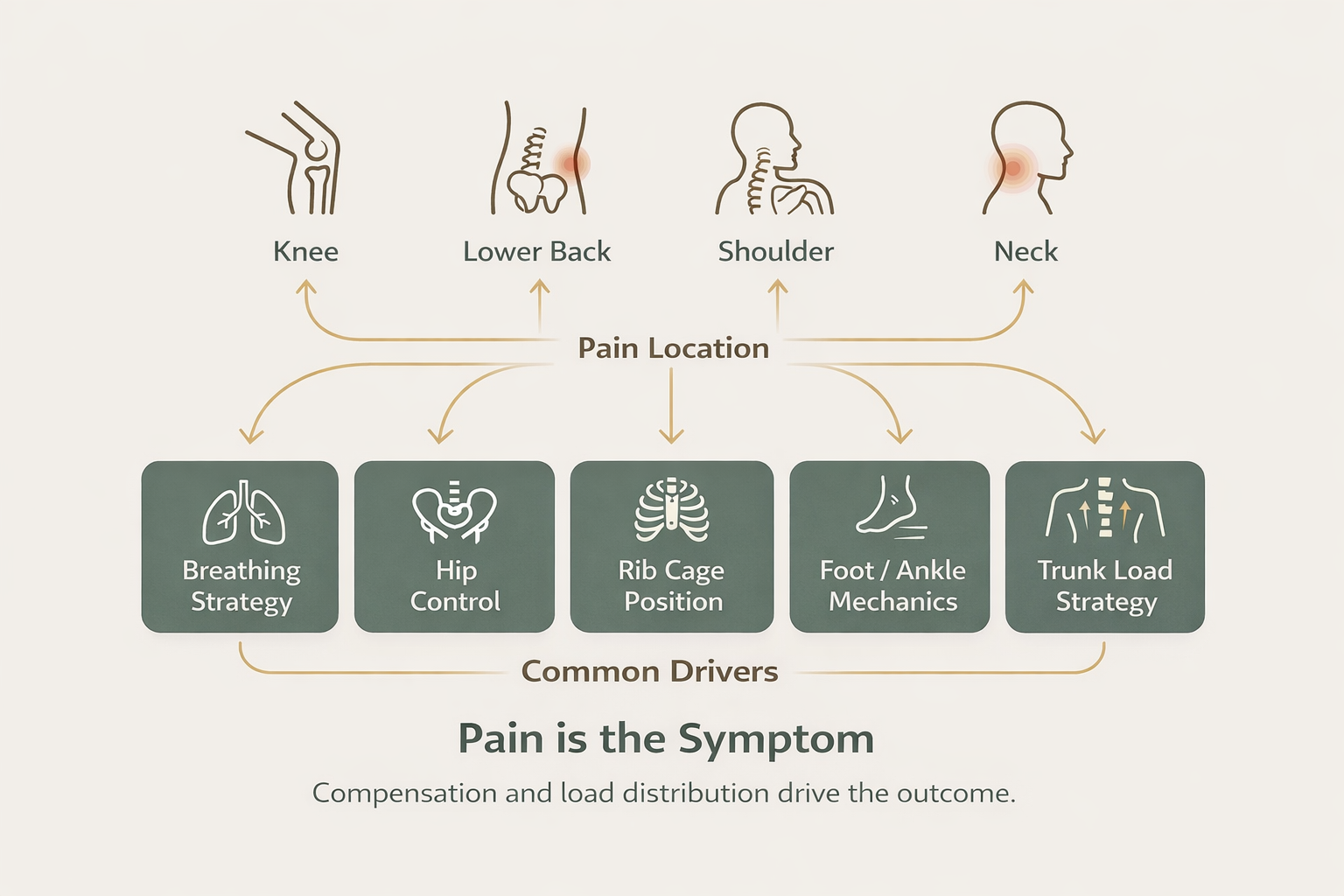
Most chronic pain doesn't come from isolated injuries. It comes from how your body distributes load and manages movement. And when that system breaks down, pain shows up at the weakest link—not necessarily where the breakdown started.
This is how we approach movement assessment at Unified Health & Fitness in Toronto: pain is the symptom, compensation is the cause.
Why Pain Keeps Moving (Or Coming Back)
Acute injuries usually have obvious causes: you twisted your ankle, lifted something awkwardly, or collided with something.
But recurring pain works differently.
It improves with rest, then returns when you resume normal activity. Or it shifts—your back feels better but now your knee is acting up. Or it flares during activities that shouldn't be related at all.
Example: A 48-year-old executive comes in with recurring lower back pain. Physiotherapy helped twice. Yoga and stretching provide temporary relief. But every time he ramps up training or has a stressful work week, the pain returns.
That's not a fragile back. That's a movement pattern the back keeps exposing.
Here's what's actually happening: the body adapted to reduce symptoms, but it didn't change the underlying strategy. The workaround works—until load, stress, or fatigue exposes it again.
Location Tells You Where It Hurts—Not Why
Pain is useful information, but it's incomplete.
What pain tells you:
Where stress is accumulating
Which tissue reached its tolerance threshold
What pain doesn't tell you:
Why that area is overloaded in the first place
Which other areas stopped contributing
How long the compensation pattern has been building
When pain keeps returning or moving around, you're not dealing with isolated tissue damage. You're dealing with a system-wide problem in how force is distributed and movement is organized.
What We Look For: Compensation, Load Distribution, Strategy
Instead of asking "What hurts?" we ask "Why is this area absorbing more stress than it should?"
This is the foundation of our assessment-based personal training approach in Etobicoke — we identify patterns, not just symptoms.
Compensation Patterns
Your body prioritizes task completion over efficiency. If one area can't contribute, another picks up the slack:
Limited hip mobility → the lower back moves more
Poor ankle control → the knee takes on extra load
Weak breathing mechanics → the neck becomes a stabilizer
These compensations feel normal until something breaks down.
Load Distribution
Pain appears where load accumulates—not where the problem started. We assess:
How force travels through joints
Which areas are absorbing impact vs. sharing it
Where stress repeatedly concentrates
Research in regional interdependence demonstrates that seemingly unrelated body regions can influence symptoms in distant locations,[1] supporting assessment beyond the site of pain.
Movement Strategy
Two people can do the same exercise and load completely different tissues. Why?
Posture, breathing, and coordination under load create entirely different stress patterns. This is why generic rehab programs often fail—they ignore individual movement strategy.
System Thinking vs. Symptom Chasing
Traditional approaches:
Identify the painful structure
Treat it locally
Hope it holds
This works for acute injuries. For chronic pain? Not so much.
Research validates this approach: studies show that pathoanatomic (location-based) diagnosis has limited utility for mechanical low back pain, while movement system impairment classification—based on how the body organizes movement—provides more clinically useful categories.
Our Toronto-based assessment process examines:
How you stand, breathe, and organize movement
How joints interact under actual load
Where control breaks down—not just where pain appears
We're tracking patterns that repeat across different activities and stress levels. Because recurring pain almost always means the same flawed strategy is being used repeatedly.
The Cycle That Keeps People Stuck
You've tried physiotherapy. Stretching. Strengthening exercises targeting the painful area.
The pain improves. Then it comes back.
Here's why: treatment stopped once symptoms improved, but the underlying movement strategy never changed.
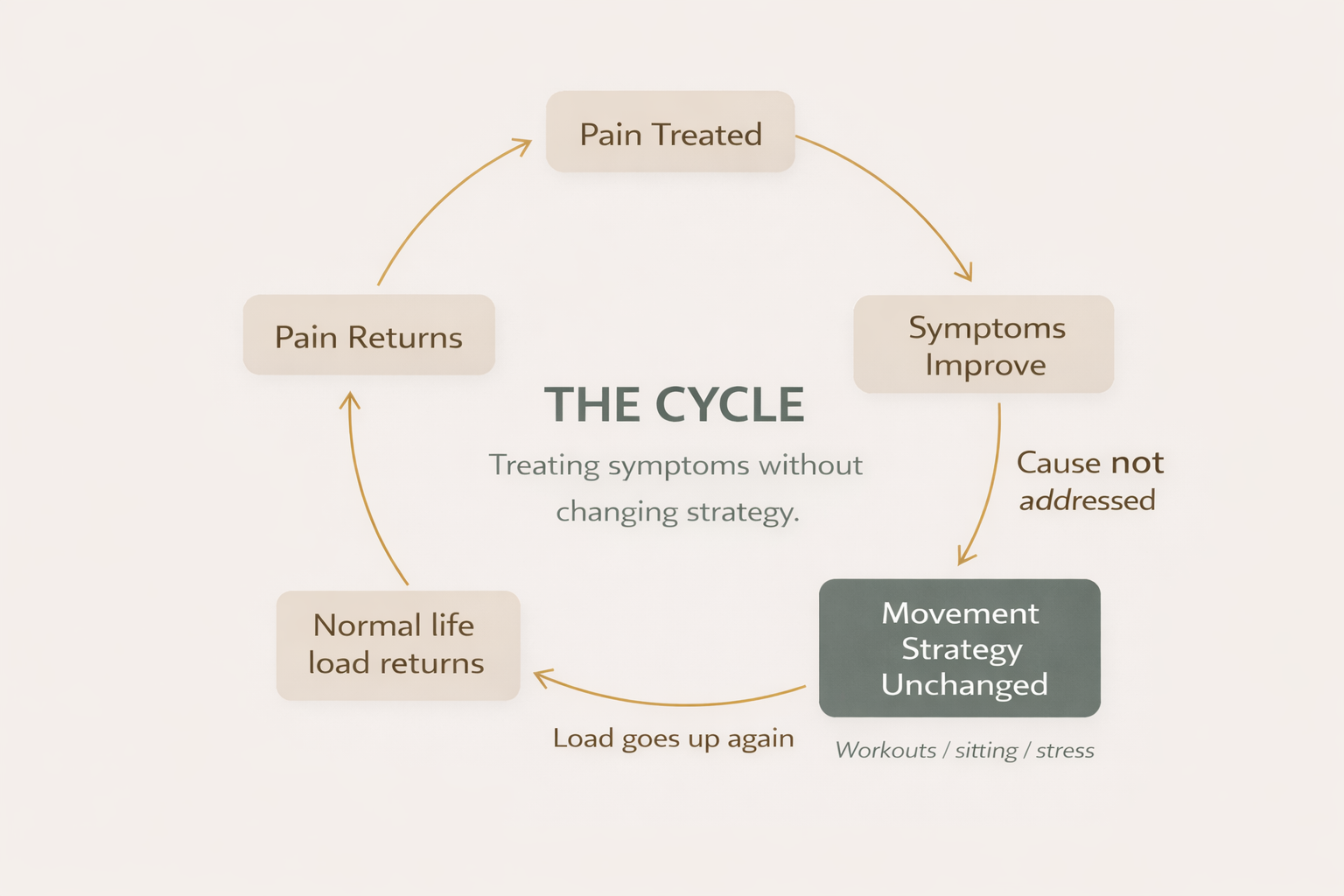
The cycle:
Pain fades with treatment
Compensation pattern remains
Load increases again
Pain returns
Breaking this cycle requires identifying and changing the pattern—not just treating the symptom.
How to Use This Series
This hub page explains the framework. The linked articles show how it applies to specific pain locations.
How to navigate:
Start here to understand why pain location misleads
Jump to the article matching your pain
Notice how often the cause originates elsewhere
Use this insight to decide if assessment makes sense for your situation
Where Pain Shows Up — and What It’s Often Compensating For
Each guide below explains common compensation patterns tied to a specific pain location — not just local symptoms.
Lower Back Pain — often a breathing, core strategy, or load management issue rather than a fragile spine
Knee Pain — commonly a load-sharing problem involving the hip or foot
Shoulder Pain — frequently tied to rib cage position, thoracic mobility, and neck mechanics
Hip Pain — the crossroads of lower-body compensation and pelvic control
Neck Pain — stress, posture, breathing, and jaw influence showing up locally
The Takeaway
Recurring pain isn't about damaged parts. It's about flawed systems.
When you address compensation patterns, load distribution, and movement strategy—instead of chasing symptoms—pain becomes useful information instead of a mystery.
If your pain keeps returning, the problem likely isn't where you think it is. And that's actually good news: systems can change.
Ready to understand your specific pattern? Book a free consultation and start with assessment, not assumptions.